“… Our study shows that percutaneous CT-guided radiofrequency ablation yields high proportions of sustained [complete responses] in properly selected patients with primary or secondary lung malignancies, and is associated with acceptable morbidity,’ write the authors.”
“Treatment options are limited for patients with non-small-cell lung cancer (NSCLC) who are not surgical candidates, and surgery is frequently not feasible for patients with secondary lung malignancies. However, according to new data published online June 17 in the Lancet Oncology, radiofrequency ablation could be an option for patients who are unable to undergo surgery, radiotherapy, or chemotherapy.
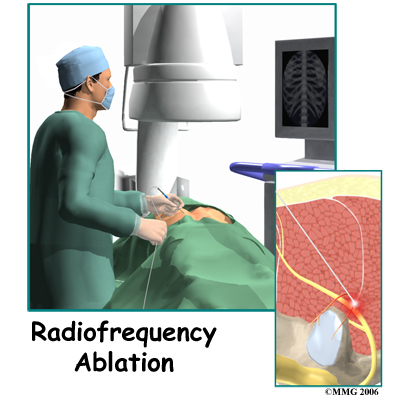 Percutaneous radiofrequency ablation is a relatively new and minimally invasive technique that has been used to treat solid tumors. In particular, it is becoming a viable option for unresectable liver malignancies. Although the use of radiofrequency ablation is at an early stage of clinical application for other types of solid tumors, recent studies have shown that it has potential in the treatment of lung, bone, and renal malignancies. The authors note that several single-institution case series have suggested that radiofrequency ablation is a feasible option for patients with unresectable or medically inoperable pulmonary tumors.
Percutaneous radiofrequency ablation is a relatively new and minimally invasive technique that has been used to treat solid tumors. In particular, it is becoming a viable option for unresectable liver malignancies. Although the use of radiofrequency ablation is at an early stage of clinical application for other types of solid tumors, recent studies have shown that it has potential in the treatment of lung, bone, and renal malignancies. The authors note that several single-institution case series have suggested that radiofrequency ablation is a feasible option for patients with unresectable or medically inoperable pulmonary tumors.
In this study, Riccardo Lencioni, MD, associate professor of radiology in the department of oncology, transplants and advanced technologies in medicine at the University of Pisa, in Italy, and colleagues designed a prospective single-group multicenter clinical trial to evaluate the feasibility, safety, and effectiveness of percutaneous computed tomography (CT)-guided radiofrequency ablation in the treatment of NSCLC. The study also included patients with metastatic disease to the lungs.
A series of 106 patients, with a total 183 lung tumors measuring 3.5 cm or smaller in diameter, were enrolled in the study. Of this group, 33 patients had been diagnosed with NSCLC, 53 had metastasis from colorectal carcinoma, and 20 patients had metastasis from other primary malignancies. All of the patients were deemed unsuitable for surgery, radiotherapy, or chemotherapy.
The primary end points were technical success, safety, and confirmed complete response of tumors. The authors defined technical success as the correct placement of the ablation device in all target tumors with completion of the planned ablation protocol. Secondary end points of the study included overall survival, cancer-specific survival, and quality of life.
Study participants underwent radiofrequency ablation in accordance with standard rules for CT-guided lung biopsy. Follow-up visits were scheduled at 1 and 3 months after the procedure, and then at 3-month intervals for up to 2 years.
A total of 137 procedures were performed, and treatment was successfully completed in 105 of 106 patients (99%). From this group, it was possible to assess the primary end point of a confirmed complete response in 85 patients (80%). The researchers noted a confirmed complete response of all targeted tumors that lasted for at least 1 year after treatment in 75 of 85 patients (88%), with incomplete ablation and evidence of local progression in at least 1 treated tumor in the remaining patients. There was no difference in tumor responses to ablation between patients with NSCLC and those with metastatic lung disease.
Overall and Cancer-Specific Survival
| Patient Subgroup |
Overall Survival at 1 Year |
Overall Survival at 2 Years |
Cancer-Specific Survival at 1 Year |
Cancer-Specific Survival at 2 Years |
| NSCLC |
70% |
48% |
92% |
73% |
| Stage 1 NSCLC |
n/a |
75% |
n/a |
92% |
| Colorectal metastases |
89% |
66% |
91% |
68% |
| Metastases from other sites |
92% |
64% |
93% |
67% |
Although there was no procedure-related mortality, 27 of the procedures were complicated by a large or symptomatic pneumothorax that required drainage. A second major complication was the occurrence of pleural effusion in 4 procedures, which also necessitated drainage.
‘Our study shows that percutaneous CT-guided radiofrequency ablation yields high proportions of sustained [complete responses] in properly selected patients with primary or secondary lung malignancies, and is associated with acceptable morbidity,’ write the authors.
They note that the rate of overall survival was greatly affected by the recruitment of patients with severely impaired pulmonary function, with substantial comorbidities, or both. All participants were deemed unsuitable for surgery, radiotherapy, or chemotherapy, or they had exhausted conventional treatment options. Under these circumstances, it was not possible to reliably compare radiofrequency ablation survival curves and those achieved with other treatments.
‘Additionally, the patient population was heterogeneous and included patients with NSCLC and patients with pulmonary metastases from different primary malignancies, and the study was not designed to provide evidence of survival benefits,’ they write. ‘A randomized controlled trial comparing radiofrequency ablation versus standard treatment options is now warranted to prove the clinical benefit of this approach.’”
[Quoted Source: Radiofrequency Ablation Offers Promise in Treatment of Lung Cancer (access requires free Medscape registration), by Roxanne Nelson, Medscape Medical News, MedscapeToday, June 19, 2008 (summarizing the Lancet Oncology article entitled, Response to radiofrequency ablation of pulmonary tumours: a prospective, intention-to-treat, multicentre clinical trial (the RAPTURE study); Lencioni, R. et. al., Lancet Oncology DOI:10.1016/S1470-2045(08)70155-4 (early publication on-line), June 18, 2008).
Comment: The Lancet study findings indicate that radiofrequency ablation is a fairly safe and very effective treatment for lung metastases up to 3.5 cm in size. Importantly, the Lancet study findings indicate that there was no difference in tumor response to ablation between patients with primary lung cancer and those with secondary metastatic lung disease caused by another form of cancer originating outside of the lungs. Any women with ovarian cancer metastatic lung disease should show this study to her doctor to determine if she is eligible for radiofrequency ablation. As noted under the “Additional Studies, Clinical Trials & Other Information” section below, a 2007 U.S. study found pulmonary radiofrequency ablation for inoperable lung cancer safe and effective. Moreover, a 2006 U.S. study found radiofrequency ablation safe and effective for the treatment of ovarian cancer metastasis. Accordingly, percutaneous radiofrequency ablation can be effective in the treatment of ovarian cancer metastatic lung and liver disease for select women.
Additional Studies, Clinical Trials & Other Information:
- Radiofrequency Ablation of Lung Tumors, RadiologyInfo.org, February 4, 2008.
- For Open Radiofrequency Ablation Clinical Trials Enrolling Patients with Lung Metastases, click here.
- Radiofrequency Ablation Effective Treatment For Inoperable Lung Cancer, Science News, ScienceDaily.com, March 28, 2007 (summarizing the findings of Pulmonary radiofrequency ablation: long-term safety and efficacy in 153 patients; Simon, C.J. et. al., Radiology. 2007 Apr;243(1):268-75).
- Early Results Indicate Radiofreqency Ablation Useful In Treating Ovarian Cancer Metastasis, Science News, ScienceDaily.com, October 9, 2006 (summarizing the findings of Percutaneous radiofrequency ablation of ovarian cancer metastasis to the liver: indications, outcomes, and role in patient management; Gervais, D.A., et. al., AJR Am J Roentgenol, 2006 Sep;187(3):746-50).
- FDA Public Health Notification: Deaths reported following Radio Frequency Ablation of Lung Tumors, U.S. Food & Drug Administration/Center For Devices & Radiological Health, December 11, 2007.
- To obtain a copy of the Phase II Clinical Trial protocol (entitled, Radiofrequency Ablation of Pulmonary Tumors Response Evaluation: a Prospective, Intention-to-Treat, Multicenter Clinical Trial) underlying the completed study above, click here.
 Yesterday, Libby’s H*O*P*E* added a new cancer video archive to the weblog courtesy of Vodpod.com. Currently, the archive contains approximately 90 videos that address many general cancer and ovarian cancer issues, as well as the personal voices of those affected by cancer. The new video archive is located on the homepage right sidebar. All you have to do is “click and play.” The video arrangement is set to “random order” so that new videos appear on the homepage sidebar each time you visit Libby’s H*O*P*E*.
Yesterday, Libby’s H*O*P*E* added a new cancer video archive to the weblog courtesy of Vodpod.com. Currently, the archive contains approximately 90 videos that address many general cancer and ovarian cancer issues, as well as the personal voices of those affected by cancer. The new video archive is located on the homepage right sidebar. All you have to do is “click and play.” The video arrangement is set to “random order” so that new videos appear on the homepage sidebar each time you visit Libby’s H*O*P*E*.