An analysis conducted by Ohio State University cancer researchers found that adding the targeted therapy bevacizumab to the first-line treatment of patients with advanced ovarian cancer is not cost effective.
An analysis conducted by Ohio State University cancer researchers found that adding the targeted therapy bevacizumab [Avastin®] to the first-line treatment of patients with advanced ovarian cancer is not cost-effective.
The findings comparing the relative value of various clinical strategies were published online March 7 in the Journal of Clinical Oncology (JCO).

Dr. David E. Cohn is a gynecologic oncologist & researcher at The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital & Richard J. Solove Research Institute. He is also the lead author of the bevacizumab cost-effectiveness study.
The researchers performed a cost-effectiveness analysis looking at a clinical trial conducted by the Gynecologic Oncology Group (GOG) studying the use of bevacizumab along with standard chemotherapy for patients with advanced ovarian cancer, said first author Dr. David E. Cohn, a gynecologic surgical oncologist and researcher at The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James).
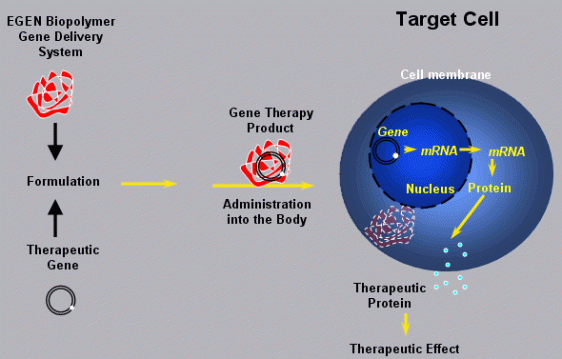
Bevacizumab is a novel targeted therapy designed to inhibit angiogenesis, the process by which new blood vessels develop and carry vital nutrients to a tumor.
Although a discussion regarding cost-effectiveness of a potentially life-extending intervention invariably suggests the rationing of limited health care resources, the intent of this study was to provide a framework with which to evaluate the pending results of a clinical trial of three different interventions for ovarian cancer, said Cohn.
“We do not suggest that bevacizumab, also known by the brand name Avastin, should be withheld from a patient with ovarian cancer, but rather argue that studies evaluating the effectiveness of new treatments should also be interpreted with consideration of the expense,” says Cohn, who collaborated with Dr. J. Michael Straughn Jr., an associate professor of obstetrics and gynecology at the University of Alabama at Birmingham.
The results of the randomized phase III [GOG 218] clinical trial demonstrated an additional 3.8 months of progression-free survival (PFS) when maintenance bevacizumab was added for about one year following treatment with standard chemotherapy drugs carboplatin and paclitaxel along with bevacizumab.
“We put together a model looking at the variety of treatment arms on this clinical trial, each of which included 600 patients,” said Cohn. “Given the fact that the addition of the drug was associated with 3.8 months of additional survival without cancer, we set out to determine whether or not that benefit of survival was justified by the expense of the drug.”
The model showed that standard chemotherapy for patients in the clinical trial would cost $2.5 million, compared to $78.3 million for patients who were treated with standard chemotherapy and bevacizumab, plus additional maintenance treatments of bevacizumab for almost one year.
Bevacizumab has been used in the treatment of recurrent ovarian cancer, and the U.S. Food and Drug Administration has approved it for the treatment of colorectal, lung, breast, brain (glioblastoma) and renal cell [kidney] cancers.
Typically each treatment with bevacizumab costs $5,000, with most of those costs directly attributable to the cost of the drug, Cohn said.
Effectiveness was defined as months of progression-free survival, and costs were calculated as total costs per strategy. Cost-effectiveness strategies were defined as the cost per year of progression-free survival. Incremental cost-effectiveness ratio was defined as the costs per progression-free year of life saved.
“Ultimately, we found that if you reduced the drug cost to 25 percent of the baseline, it does become cost effective to treat patients with bevacizumab,” said Cohn. “Or, if the survival could be substantially increased above the 3.8 months of progression-free survival, that could lead to cost-effective treatment for patients with advanced ovarian cancer.”
Ovarian cancer is the most lethal gynecologic cancer, with almost 14,000 women expected to die from the disease this year, according to the American Cancer Society.
“It is anticipated that in the future, there will be increased scrutiny regarding the individual and societal costs of an effective medication,” said Cohn. “We hope that future clinical trials will incorporate the prospective collection of cost, toxicity and quality-of-life data to allow for a fully informed interpretation of the results.”
Other Ohio State researchers involved in the study are Kenneth H. Kim, Kimberly E. Resnick and David O’Malley.
Big Cost For Little Gain in Ovarian Cancer – JCO Editorial
Results of the cost-effectiveness model reported above by Cohen et. al. reveal that paclitaxel plus carboplatin plus bevacizumab, followed by bevacizumab maintenance (PCB-B), as tested in the GOG 218 phase III clinical trial, costs $78.3 million ($1,305,000 per patient) with an incremental cost-effectiveness ratio of $401,088 per progression-free year of life saved. It is important to note that traditional cost-effectiveness study models utilize the costs of improvements in overall survival, as compared to the traditional cost-effective standard of $50,000 per year of life saved, or more recently, $100,000 per year of life saved. Cohen et. al. found that the traditional standard of $100,000 per progression free year of life saved can be achieved in calculating the incremental cost-effectiveness ratio, but only at a bevacizumab drug price point that is 25% below the actual drug cost.

Martee L. Hensley, M.D., Gynecologic Medical Oncology Service, Memorial Sloan-Kettering Cancer Center
In an accompanying JCO editorial, Martee L. Hensley, M.D., a board-certified medical oncologist who treats women with gynecologic cancers at the Memorial Sloan-Kettering Cancer Center in New York city, raises several important considerations with respect to the Ohio State University study.
First, Dr. Hensley notes that the “costs” accounted for by the Ohio State University researchers only refer to the additional monies incurred by adding bevacizumab to the standard of care paclitaxel-carboplatin treatment. Specifically, the researchers used a standard cost metholodolgy based upon estimates of drug costs using Medicare reimbursement rates. The model used does not include indirect costs (e.g., patient out-of-pocket expenses, time lost from work associated with 51 weeks of bevacizumab maintenance, etc.). The only costs related to toxicity of treatment included by researchers were those associated with management of intestinal perforations. Dr. Hensley highlights the fact that the cost model does not include management of grade 2 or worse hypertension or other potential problems that may be caused by bevacizumab or the other chemotherapy drugs. To the extent that additional costs are added to the model, the cost-effectiveness ratio generated by the researchers would worsen.
Second, Dr. Hensley explains that out of necessity, the researchers’ cost-effectiveness model used PFS data due to the unavailability of overall survival or quality adjusted overall survival data in connection with the three most recent bevacizumab phase III clinical trials. This model construct assumes that the 3.8 month improvement in PFS (as reported by the GOG 218 trial investigators) provides an improvement in the patient’s experience. Dr. Hensley emphasizes that most ovarian cancer recurrences are identified while the patient is still asymptomatic, with the help of CA-125 blood testing and computed tomography imaging (i.e., CT scan). Stated differently, it may not be correct to assume that remaining radiographically progression-free for an addtional 3.8 months would improve a patient’s quality of life. If GOG 218 ultimately finds that PCB-B does not improve overall survival, then the drug’s cost-effectiveness will drift farther away from an acceptable level, says Hensley.
Third, Dr. Hensley points out that only when PFS associated with PCB-B use was hypothetically extended to 32.1 months (observed PFS in GOG 218 was 14.1 months) by the researchers did the incremental cost-effectiveness ratio approach $100,000 per progression-free year of life saved. Hensley believes that the bevacizumab data accrued to date suggests that a 32.1 month PFS is unlikely. Notably, median PFS is only 24 months among lower-risk patients with optimally debulked stage III ovarian cancer treated with intraperitoneal-based platinum drug/taxane drug therapy.
Fourth, Dr. Hensley explains that it may be possible to achieve a better incremental cost-effectiveness ratio based upon preliminary data derived from the Gynaecologic Cancer Intergroup (GCIG) phase III randomized clinical trail of paclitaxel plus carboplatin, with or without bevacizumab and bevacizumab maintenace therapy (ICON7 trial). The bevacizumab dose tested in ICON7 was only half of that used in GOG 218 (7.5 mg/kg versus 15 mg/kg), and the duration of maintenance therapy in ICON7 was only 36 weeks of continued treatment as compared to 51 weeks in GOG 218. Preliminary results reported by the GCIG in ICON7 indicate that bevacizumab creates a PFS advantage in line with that produced in GOG 218, but at half the dose. Based on these facts, Hensley states that potential use of lower-dose and shorter-duration bevacizumab would improve the incremental cost-effectiveness ratio. Moreover, if lower dose/shorter duration bevacizumab use is also found to reduce the frequency of grade 2 or worse hypertension, the overall costs associated with the drug would also be lower, says Hensley.
Dr. Hensley believes that there are additional steps to be taken (and questions to be answered) which could improve an evaluation of the role and costs of bevacizumab:
- Is there a clinically meaningful overall survival advantage to PCB-B over paclitaxel plus carboplatin? If PCB-B is not effective, then by definition, it is not cost-effective.
- Is the data from ICON7 sufficient to permit treatment at half the dose for 9 months instead of 12 months? If so, total bevacizumab costs would be lower.
- Is there a subset of patients who benefit dramatically from PCB-B?
- If there is a subset of patients who benefit dramatically from PCB-B, it is necessary to study this group of women to determine if potential biomarkers can identify which patients will or will not benefit from the addition of bevacizumab. Identifying biomarkers that can predict response means commitment to correlative studies as part of large clinical trials.
In sum, Dr. Hensley believes that buying bevacizumab at $78.3 million for 3.8 months of progression-free survival on behalf of approximately 600 women is not sustainable in today’s health care delivery system. Moreover, the incurrence of such costs may hinder basic clinical research to find better compounds that improve PFS by a more meaningful magnitude, says Dr. Hensley. From Hensley’s perspective, it appears that the stage is set for a potential collision between medicine and policy with respect to where and how a finite number of health care dollars will be spent.
About the Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute
The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (cancer.osu.edu) is one of only 40 Comprehensive Cancer Centers in the United States designated by the National Cancer Institute. Ranked by U.S. News & World Report among the top cancer hospitals in the nation, The Arthur G. James Hospital is the 205-bed adult patient-care component of the cancer program at The Ohio State University. The OSUCCC – James is one of only seven funded programs in the country approved by the NCI to conduct both phase I and II clinical trials.
Sources:
- Cohn DE, Kim KH, Resnick KE, et. al. At What Cost Does a Potential Survival Advantage of Bevacizumab Make Sense for the Primary Treatment of Ovarian Cancer? A Cost-Effectiveness Analysis. J. Clin. Oncol. (JCO.2010.32.1075); published online before print on March 7, 2011.
- Ohio State Study: Targeted Ovarian Cancer Therapy Not Cost-Effective, Press Release, The Ohio State University Comprehensive Cancer Center–Arthur G. James Cancer Hospital and Solove Research Institute, March 7, 2011.
- Hensley M. Big Costs for Little Gain in Ovarian Cancer. J. Clin. Oncol., published online before print March 7, 2011, doi: 10.1200/JCO.2010.34.0489. (Adobe Reader PDF document).
- Burger RA, Sill MW, Monk BJ, et. al. Phase II trial of bevacizumab in persistent or recurrent epithelial ovarian cancer or primary peritoneal cancer: a Gynecologic Oncology Group Study [GOG 218]. J Clin Oncol. 2007 Nov 20;25(33):5165-71. PubMed PMID: 18024863.
- Perren T, Swart AM, Pfisterer J, et. al. ICON7: A phase III randomized gynecologic cancer intergroup trial of concurrent bevacizumab and chemotherapy followed by maintenance bevacizumab, versus chemotherapy alone in women with newly diagnosed epithelial ovarian (EOC), primary peritoneal (PPC), or fallopian tube cancer (FTC). Ann Oncol 21;viii2, 2010 (suppl 8; abstr LBA4).