Caris Life Sciences announces the launch of a new molecular profiling service for ovarian cancer patients
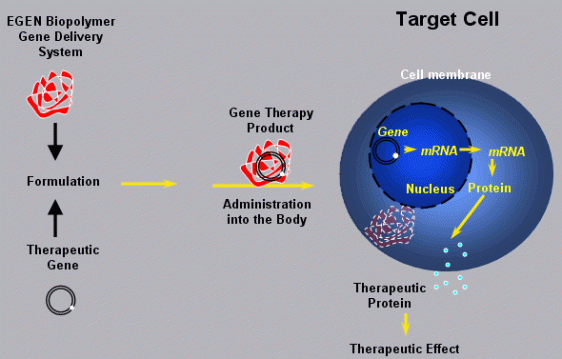
Caris Life Sciences, Inc. (Caris), a leading biosciences company focused on enabling precise and personalized healthcare through the highest quality anatomic pathology, molecular profiling, and blood-based diagnostic services, announced the launch of a new, Caris Target Now™ molecular profile for ovarian cancer patients. This expansion of the Caris Target Now™ offering provides individualized molecular information to treating physicians, relevant to the selection of therapies to treat this highly-lethal cancer. Ovarian cancer affects more than 20,000 women annually and produces some of the highest five-year mortality rates found among the 200+ types of cancer.
Caris Target Now™ molecular profiling examines the unique genetic and molecular make-up of each patient’s tumor so that treatment options may be matched to each patient individually. Caris Target Now™ helps patients and their treating physicians create a cancer treatment plan based on the tumor tested. By comparing the tumor’s information with data from published clinical studies by thousands of the world’s leading cancer researchers, Caris can help determine which treatments are likely to be most effective and, just as important, which treatments are likely to be ineffective.
The Caris Target Now™ test is performed after a cancer diagnosis has been established and the patient has exhausted standard of care therapies or if questions in therapeutic management exist. Using tumor samples obtained from a biopsy, the tumor is examined to identify biomarkers that may have an influence on therapy. Using this information, Caris Target Now™ provides valuable information on the drugs that will be more likely to produce a positive response. Caris Target Now™ can be used with any solid cancer such as lung cancer, breast cancer, prostate cancer, and now, ovarian cancer.
Evidence Behind Caris Target Now™

Daniel D. Von Hoff, M.D., F.A.C.P., is the Executive Director of Caris Life Sciences' Clinical Research
A multi-center, prospective, pilot study first published in The Journal of Clinical Oncology (JCO) in October 2010 [1] — along with an accompanying editorial [2] — determined that personalized cancer treatment tailored to a tumor’s unique genetic make-up identified therapies that increased progression free survival (PFS) over previous therapies in 27% of patients with advanced disease.
The purpose of the study was to compare PFS using a treatment regimen based on the molecular profiling (MP) of a patient’s tumor with the PFS determined for the most recent regimen on which the patient had experienced progression after taking that regimen for 6 weeks. Unlike a typical control study, each patient was his or her own study control. Tissue samples from patients with refractory metastatic cancer were submitted for MP in two formats including:�
In many of these refractory tumors, targets for conventional therapies were identified, which was “a surprise finding,” according to Dr. Daniel Von Hoff, the Executive Director of Caris’ Clinical Research. But the profiling also suggested therapies in cases where the treating physician was unsure regarding the next line of treatment. The MP approach was found to have clinical benefit for the individual patient who had a PFS ratio (PFS on MP selected therapy/PFS on prior therapy) of ≥ 1.3. Among the 86 patient tumors that were profiled with Caris Target Now™:
- �84 (98%) had a detected molecular target;
- �66 of the 84 patients were treated with therapies that were linked to their MP results; and
- 18 (27%) of 66 patients had a PFS ratio of ≥ 1.3 (95% CI, 17% to 38% range; one-sided, one-sample P = .007).
The study investigators concluded that it is possible to identify molecular targets in patients’ tumors. In 27% of the patients, the MP approach resulted in a longer PFS on a MP-based regimen than on the regimen that was based on physician’s choice. “It was also encouraging to see that the overall survival in these 18 patients was better than that for the whole group of 66 patients (9.7 vs. 5 months),” said Von Hoff.
Of the 66 participants, 27% had breast cancer, 17% had colorectal cancer, and 8% had ovarian cancer; the remainder were classified as miscellaneous. The improvement in PFS among the various types of cancer patients was as follows: 44% in patients with breast cancer, 36% in those with colorectal cancer, 20% in those with ovarian cancer, and 16% in the miscellaneous group.
The investigators in the study utilized Caris Target Now™ molecular profiling, which is currently available to oncologists and their patients.
“Oncologists commonly expect a 1-in-20 chance of patient response in 3rd- and 4th-line therapies. This recent study suggests those odds can be improved to 1-in-4 when using therapeutic guidance provided by Caris Target Now™.”
— Dr. Jeff Edenfield, a practicing oncologist with US Oncology, and routine user of Caris Target Now™
Since 2008, more than 15,000 cancer patients have received a Caris Target Now™ molecular profile. Caris Target Now™ has been designed to provide treating physicians with therapeutic options, often identifying anti-tumor agents that may not have been considered before. The Caris Target Now™ report is based on the genetic make-up of an individual patient’s tumor cross-referenced with a vast and growing proprietary database of clinical literature, correlating genetic tumor information to therapeutic response. Using biomarker-based therapies has been linked to the likelihood of a positive patient response.

James H. Doroshow, M.D., Director, Division of Cancer Treatment & Diagnosis, National Cancer Institute
In the accompanying JCO editorial, James H. Doroshow, M.D., the Director of the National Cancer Institute (NCI) Division of Cancer Treatment and Diagnosis, commented that the study by Von Hoff et. al. possessed several limitations. [2] The stated limitations of the study include (i) uncertainty surrounding the achievement of the study’s primary end point based upon use of the time-to-disease progression (TTP) index; (ii) limited prior experience with patients as their own controls, and (iii) lack of study randomization. Despite these limitations, Dr. Doroshow noted that important lessons can be learned from the study conducted by Von Hoff et. al.
“First and foremost, this study vividly reminds us that the need for therapeutic intervention arises one patient at a time. When we sit with an individual who is trying to live with an advanced solid tumor after having already received several different chemotherapy regimens, it is unlikely that any published prognostic index or gene signature, as currently implemented, will be of much help in decision making—for physicians or for patients. [citation omitted]. Thus, a truly urgent need exists to move past the empiric therapeutic paradigm that launched the first half century of systemic oncologic treatment. [citation omitted]. Von Hoff et al have taken a noteworthy, albeit somewhat flawed, first step in this direction in their attempt to imagine a novel paradigm for cancer therapy, using the techniques of molecular tumor characterization on an individual patient basis. Future investigators of new cancer therapies should learn from this initial effort and focus on how these rapidly evolving molecular tools can be used in the development of an entirely new investigative model for the systemic treatment of cancer.”
Caris is currently conducting and initiating additional studies of Caris Target Now™ molecular tumor profiling through collaboration with leading institutions and cancer centers. �
With 300% growth in utilization in 2010, medical oncologists are recognizing the utility and value of this novel approach in providing improved care to patients. Physician adoption is rapidly accelerating, as Caris recently reached the threshold of providing Caris Target Now™ services to more than 1,000 patients per month. This new introduction for ovarian cancer is most relevant for physicians treating women who have progressed on platinum-based therapy and/or who need guidance for third-line treatment options. Caris Target Now™ for ovarian cancer offers the opportunity for these women to benefit from personalized and targeted therapy guidance based upon molecular profiling.
“Ovarian cancer is a highly-lethal cancer that presents distinct diagnostic and therapeutic challenges, often presenting no major symptoms until the cancer has metastasized,” said Dr. Les Paul, Caris’ Senior Vice President for Medical Affairs. “Choosing the optimal therapeutic intervention at the earliest possible stage is critical to extending progression free survival in ovarian cancer patients. With the introduction of the Caris Target Now™ ovarian profile, we are able to support physicians with as much information as possible, including the latest relevant clinical literature citations to aid them in making the best therapeutic decision possible for each patient.”
Examples of the potential use of an existing clinical trial drug to target a specific molecular characteristic possessed by an ovarian cancer include:
Use of Molecular Profiling By Leading Medical Institutions; Sponsorship By A Charitable Foundation
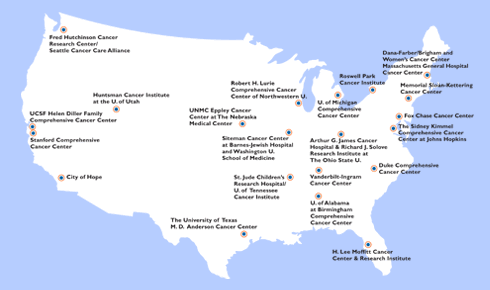
It should be noted that molecular profiling is already being used in clinical practice at several leading cancer institutions. At Massachusetts General Hospital, (MGH), The MGH Cancer Centre uses a PCR-based mutation-detection assay and state-of-the-art robotic technology, called “SNaPshot,” to look for 130 known gene mutations in tumor tissue. “We are already using molecular profiling for all our lung cancer patients,” said Jeffrey Settleman, Ph.D., scientific director at the MGH Cancer Center, to Medscape Oncology in 2009. [12] “This has already had an impact on treatment decisions, and it appears to be improving treatment. We have seen better response rates and we hope that this will translate into better survival.” In fact, MGH is engaged currently in the largest study aimed at matching tumor genomes to potential anticancer treatments. [13] It is our understanding that MGH performs molecular profiling currently on melanoma, leukemia, brain and metastatic breast cancer, and metastatic adenocarcinoma that start in the lung, colon or rectum.
Several other institutions are in the process of developing or have developed their own systems, including the University of Texas M.D. Anderson Cancer Center [14], and the Dana-Farber Cancer Institute [15]. All are striving to profile individual tumors so that therapy can be personalized, which means that it has a better chance of working because it targets specific mutations found in a patient’s tumor. The MP approach also prevents patients from being exposed to drugs that have a limited chance of success, eliminating toxicity and improving quality of life.
We should also note the Clearity Foundation sponsors molecular profiling services on behalf of ovarian cancer patients at no cost. The Clearity Foundation is a 501(c)(3) not-for-profit, founded by Laura Shawver, Ph.D., who is an ovarian cancer survivor and research scientist. The Clearity Foundation seeks to improve treatment outcomes in recurrent and progressive ovarian cancer patients by providing diagnostic services that determine the molecular profile of the individual patient with the belief that a molecular “blueprint” is crucial to finding appropriate treatments.
About Caris Target Now™
Caris Target Now™ is a comprehensive tumor analysis coupled with an exhaustive clinical literature search, which matches appropriate therapies to patient-specific biomarker information to generate an evidence-based treatment approach. Caris Target Now™ testing provides information that may help when considering potential treatment options.
Caris Target Now™ begins with an immunohistochemistry (IHC) analysis. An IHC test measures the level of important proteins in cancer cells providing clues about which therapies are likely to have clinical benefit and then what additional tests should be run.
If there is access to a frozen sample of patient tissue available, Caris may also run a gene expression analysis by microarray. The microarray test looks for genes in the tumor that are associated with specific treatment options.
As deemed appropriate based on each patient, Caris will run additional tests. Fluorescent In-Situ Hybridization (FISH) is used to examine gene copy number variation (i.e., gene amplification) in the tumor. Polymerase Chain Reaction (PCR) or DNA sequencing is used to determine gene mutations in the tumor DNA.
Caris takes the results from each test and applies the published findings from thousands of the world’s leading cancer researchers. Based on this analysis, Caris Target Now™ identifies potential therapies for patients and their treating physicians to discuss.
Caris Target Now™ was developed and its performance characteristics were determined by Caris, a CLIA-certified medical laboratory in compliance with the U.S. Clinical Laboratory Amendment Act of 1988 and all relevant U.S. state regulations. It has not been approved by the United States Food and Drug Administration.
About Caris Life Sciences
Caris Life Sciences, a leading biosciences company, specializes in the development and commercialization of the highest quality anatomic pathology, molecular profiling, and blood-based diagnostic technologies, in the fields of oncology, dermatopathology, hematopathology, gastrointestinal pathology and urologic pathology. The company provides academic-caliber consultations for patients every day, through its industry-leading team of expert, subspecialty pathologists. Caris also offers advanced molecular analyses of patient samples through prognostic testing services and genomic, transcriptomic, and proteomic profiling to assist physicians in their treatment of cancer. Currently, Caris is developing the Carisome™ platform, a proprietary, blood-based technology for diagnosis, prognosis, and theranosis of cancer and other complex diseases. The company is headquartered in the Dallas metroplex, and operates laboratories at the headquarters, as well as in the Phoenix and Boston metro areas.
About Daniel Von Hoff, M.D., FACP, Executive Director, Caris Life Sciences Clinical Research
Daniel D. Von Hoff, M.D., is currently physician-in-chief and director of translational research at Translational Genomics Research Institute (TGen) in Phoenix, Arizona. He is also chief scientific officer for US Oncology and the Scottsdale Healthcare’s Clinical Research Institute. He holds an appointment as clinical professor of medicine at the University of Arizona College of Medicine.
Dr. Von Hoff’s major interest is in the development of new anticancer agents, both in the clinic and in the laboratory. He and his colleagues were involved in the beginning of the development of many of the agents now in routine use, including: mitoxantrone, fludarabine, paclitaxel, docetaxel, gemcitabine, irinotecan, nelarabine, capecitabine, lapatinib and others.
At present, Von Hoff and his colleagues are concentrating on the development of molecularly targeted therapies particularly for patients with advanced pancreatic cancer. Dr. Von Hoff’s laboratory interests and contributions have been in the area of in vitro drug sensitivity testing to individualize treatment for the patient, mechanisms of gene amplification, particularly of extrachromosomal DNA, and understanding of and targeting telomere maintenance mechanisms. His laboratory work now concentrates on the discovery of new targets in pancreatic cancer.
Dr. Von Hoff has published more than 543 papers, 133 book chapters, and more than 956 abstracts. Dr. Von Hoff also served on President Bush’s National Cancer Advisory Board from June 2004 through March 2010.
Dr. Von Hoff is the past president of the American Association for Cancer Research(AACR) (the world’s largest cancer research organization), a fellow of the American College of Physicians, and a member and past board member of the American Society of Clinical Oncology (ASCO). He is a founder of ILEX™ Oncology, Inc. (acquired by Genzyme after Ilex had 2 agents, alemtuzumab and clofarabine approved for patients with leukemia). He is founder and the editor emeritus of Investigational New Drugs – The Journal of New Anticancer Agents; and, editor-in-chief of Molecular Cancer Therapeutics. He is also proud to have been a mentor and teacher for multiple medical students, medical oncology fellows, graduate students, and post-doctoral fellows. He is a co-founder of the AACR/ASCO Methods in Clinical Cancer Research Workshop.
References:
1/ Von Hoff DD, Stephenson JJ Jr, Rosen P, et. al. Pilot study using molecular profiling of patients’ tumors to find potential targets and select treatments for their refractory cancers. J Clin Oncol. 2010 Nov 20;28(33):4877-83. Epub 2010 Oct 4. PubMed PMID: 20921468.
2/ Doroshow JH. Selecting systemic cancer therapy one patient at a time: Is there a role for molecular profiling of individual patients with advanced solid tumors? J Clin Oncol. 2010 Nov 20; 28(33):4869-71. Epub 2010 Oct 4. PMID: 20921466.
3/Addition of Dasatinib (Sprycel) to Standard Chemo Cocktail May Enhance Effect in Certain Ovarian Cancers, by Paul Cacciatore, Libby’s H*O*P*E*™, April 19, 2009.
4/UCLA Researchers Significantly Inhibit Growth of Ovarian Cancer Cell Lines With FDA-Approved Leukemia Drug Dasatinib (Sprycel®), by Paul Cacciatore, Libby’s H*O*P*E*™, November 11, 2009.
5/BMS-345541 + Dasatinib Resensitizes Carboplatin-Resistant, Recurrent Ovarian Cancer Cells, by Paul Cacciatore, Libby’s H*O*P*E*™, July 1, 2010.
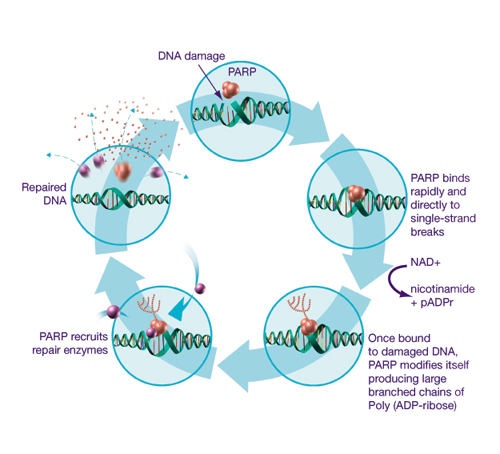
6/PARP Inhibitor Olaparib Benefits Women With Inherited Ovarian Cancer Based Upon Platinum Drug Sensitivity, by Paul Cacciatore, Libby’s H*O*P*E*™, April 23, 2010.
7/ Fong PC, Boss DS, Yap TA, et al. Inhibition of poly(ADP-ribose) polymerase in tumors from BRCA mutation carriers. N Engl J Med. 2009 Jul 9;361(2):123-34. Epub 2009 Jun 24. PMID: 19553641.
8/Audeh MW, Penson RT, Friedlander M, et al. Phase II trial of the oral PARP inhibitor olaparib (AZD2281) in BRCA-deficient advanced ovarian cancer. J Clin Oncol 2009;27(supplement):p. 15S.
9/PARP Inhibitor MK-4827 Shows Anti-Tumor Activity in First Human Clinical Study, by Paul Cacciatore, Libby’s H*O*P*E*™, November 17, 2010.
10/PI3K Pathway: A Potential Ovarian Cancer Therapeutic Target?, by Paul Cacciatore, Libby’s H*O*P*E*™, November 20, 2009.
11/Endocyte’s EC145 Produces Significant Anti-Tumor Activity In Advanced Stage Chemoresistant Ovarian Cancer Patients, by Paul Cacciatore, Libby’s H*O*P*E*™, October 21, 2009.
12/Massachusetts General Hospital Cancer Center To Genetically Profile All Patient Tumors, by Paul Cacciatore, Libby’s H*O*P*E*™, March 14, 2009.
13/Largest Study Matching Genomes To Potential Anticancer Treatments Releases Initial Results, by Paul Cacciatore, Libby’s H*O*P*E*™, August 3, 2010.
14/An Initiative for Molecular Profiling in Advanced Cancer Therapy (IMPACT) Trial. A Molecular Profile-Based Study in Patients With Advanced Cancer Treated in the Investigational Cancer Therapeutics Program, University of Texas M.D. Anderson Cancer Center, ClinicalTrials.gov Identifier: NCT00851032.
15/Dana-Farber Researchers “OncoMap” The Way To Personalized Treatment For Ovarian Cancer, by Paul Cacciatore, Libby’s H*O*P*E*™, November 16, 2010.
Sources:
Additional Information: