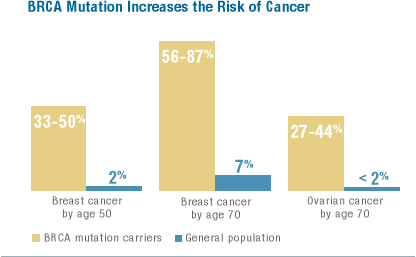
“One in 40 Ashkenazi Jews – compared to one in 500 in the general population – carries a mutation that gives women a 50 percent to 85 percent chance of getting breast cancer by the time they are 80. The genetic mutation, discovered in 1994, also increases the likelihood of melanoma and ovarian, prostate or pancreatic cancer. While within the general population about 5 percent of cancers can be attributed to a hereditary syndrome, in the Jewish community, that number is closer to 30 percent. ”
“Erika Taylor didn’t want to know whether she had the breast cancer gene.
‘My thinking was I would never get a prophylactic mastectomy,’ Taylor, 44, said of the idea of removing her breasts as a preventive measure. ‘I just thought it was horrible thing to do to myself, and if I was unwilling to do that, why bother finding out?’
Her grandmother died of breast cancer at 56, and her mother battled and beat the disease in her 30s. Taylor, who is single and the mother of a 14-year-old boy, always suspected cancer was in her future, but taking steps to confirm that was not something she wanted to do. Until she got her own diagnosis.
A routine mammogram last November revealed early stage noninvasive cancer cells in Taylor’s milk ducts, making information about her genetic status vital for determining her treatment.
All of a sudden, the idea of ‘I would never do such a thing’ goes out the window,’ she said. ‘It’s astonishing how quickly you go, ‘OK, OK, what do I need to do? I’ll do it.” Taylor’s mother tested first, and when she was identified as a carrier of the BRCA 2 genetic mutation common in Ashkenazi Jews, Taylor tested next. In January, she found out she, too, carries the gene that makes it likely that even if she were to rid herself of her diagnosed cancer, it would probably recur.
Like a growing number of women, Taylor faced both the gift and the terror of knowledge.
One in 40 Ashkenazi Jews – compared to one in 500 in the general population – carries a mutation that gives women a 50 percent to 85 percent chance of getting breast cancer by the time they are 80. The genetic mutation, discovered in 1994, also increases the likelihood of melanoma and ovarian, prostate or pancreatic cancer. While within the general population about 5 percent of cancers can be attributed to a hereditary syndrome, in the Jewish community, that number is closer to 30 percent.
The good news is that knowledge about how the mutation causes cancer is opening scientific doors to more effective, targeted treatment for those already diagnosed. And people who have the genetic mutation can take preventative measures to drastically reduce their breast and ovarian cancer risk.
Surgery – removal of the breasts and ovaries – reduces the risk of breast cancer by 90 percent, to well below the 13 percent odds of getting breast cancer in the general population. But less-drastic measures, such as drug therapy, removal of just the ovaries and careful screening to catch and cure the cancer at an early stage, can also save lives. Genetic information also helps women feel empowered to take control of other factors that raise risk, such as smoking, alcohol consumption and obesity.
‘The use of genetic information to understand a person’s risk for diseases like cancer is clearly reaping huge benefits,’ said Dr. William Audeh, a medical oncologist with an emphasis on hereditary risk at Cedars-Sinai Medical Center‘s Samuel Oschin Comprehensive Cancer Institute. ‘It’s gone from being a somewhat frightening piece of information that gave people concerns to a hugely important piece of information that empowers people to either take preventative steps that can save their lives or to accurately target therapy if one develops cancer. There is a general understanding that genetic information for cancer is going to be critical for taking the best care of people.’
Knowing she had the genetic mutation sent Taylor, editor of the trade publication, Pool and Spa magazine, into a tailspin of research and soul-searching. Treatment for DCIS (ductal carcinoma in situ) usually consists of removal of the tumor and perhaps radiation. But Taylor’s genetic status put her in a different risk category, and after hearing from four different doctors that her cancer, even if cured, would return, she opted for a double mastectomy and reconstruction. Her surgery is scheduled for May.
Taking the test
While Taylor confirmed her genetic status after a cancer diagnosis, experts encourage people to test before cancer strikes. For Ashkenazi Jews, having just one relative who has had premenopausal breast cancer warrants getting tested, according to geneticists. (For non-Jews, testing is indicated if there are two relatives.) Any history of male breast cancer or any ovarian cancer in the family also raises a red flag, as do multiple cases of melanoma or pancreatic cancer. And women who themselves have early onset breast cancer should be tested, so they can tailor their treatment and inform other family members.
In the last five years, the number of people testing for the BRCA mutation has increased by 50 percent every year, according to Myriad Genetics, which patented the blood test for BRCA about 12 years ago. About 70,000 people tested last year. Myriad recently launched an East Coast direct-marketing campaign for the test.
Of the estimated 600,000 people who carry the gene in the United States, only about 20,000 have been identified. Of those 600,000 carriers, about 150,000 are Jewish, mostly Ashkenazi. Other ethnic groups, such as French Canadians and Filipinas, also have a genetic predisposition, as do some Latina subpopulations – some of which have been traced back to having Jewish genes.
Only about 15 percent of people who test come out with positive results, though the percentage is somewhat higher among Jews. But even a negative result is not entirely reassuring, since it indicates only that the specific mutations were not found. Other as-yet-undiscovered mutations, or other genes, could also cause a heavy incidence of cancer in a family, according to Dr. Ora Gordon, director of the GenRISK adult genetics program at Cedars.
Gordon encourages anyone being tested to see a genetic counselor to get the results properly interpreted and to understand their options if they find out they are carriers.
‘When learning about this for the first time, very frequently people say to themselves, If I’m not going to have surgery, I shouldn’t get this test.” Gordon said. ‘But that would be a tremendous loss in terms of potential reassurance for people who are not carriers and for identifying people who might have a whole variety of other options that might provide very substantial risk reduction.’
Prophylactic bilateral mastectomy – or having both breasts removed before any sign of cancer – seems to be growing in popularity as an option in the United States, though hard statistics are just now being compiled.
One recent study of women with the BRCA mutation and a cancer diagnosis put the rate of mastectomy at 50 percent in the United States, the highest by far of anywhere in the world. In Israel, that number is 2 percent, Gordon said.
In Los Angeles in particular, the numbers seem to be especially high.
Gordon estimates that 65 percent to 70 percent of BRCA-positive women in Cedars’ cancer programs opt for the surgery, some immediately, some after a few years of surveillance. ‘The quantity and quality of medical options makes the surgery more attractive in big cities, and Los Angeles has a high tolerance for breast surgery,’ Gordon said. She is spearheading a study about decision-making among BRCA-positive women at Cedars’ Gilda Radner early detection program, which screens genetically high-risk women for ovarian cancer.
Gordon understands that a woman’s decision about treatment is intertwined with her relationship status, her self-image and how many family members she saw battle or succumb to cancer.
Surgery or surveillance?
‘The decision to take off your breasts is really hard. It’s a part of your body that is associated with your outward appearance, and it’s a part of who you are. It’s a part of your sex life,’ said Joi Morris, who was 41 when she learned she carried the same genetic mutation that gave her mother and grandmother breast cancer at a young age.
Morris remembers a day, not long after she found out, when she really confronted the issue as her sons, then 7 and 10, played at the beach.
‘My kids were in the water and jumping and playing and having a fabulous time, and I looked down at my breasts in my swimming suit and thought, “Oh my God, what would it be like to not have these?'” ‘It’s a seesaw of emotions,’ she said, because at the same time, ‘you wake up every morning, and you know you are at risk, and you wonder if there is something in there you can’t find.’
Morris initially opted for close surveillance – a regimen of regular mammograms, manual exams, ultrasounds and breast MRIs – the most sensitive, noninvasive screening available, used only for high-risk patients. Her first MRI revealed a lump close to her chest wall.
‘I panicked. There is no other way to put it. That lump turned out to be benign, but the whole process was so stressful for me and hard on my family. I just decided if this lump is not cancer, the next one could be,’ Morris said.
She had a prophylactic bilateral mastectomy, with immediate reconstruction. As it turned out, her surgery wasn’t prophylactic at all – pathology revealed pre-cancerous cells scattered throughout both breasts.
Early in the process, Morris turned for support and information to FORCE: Facing Our Risk for Cancer Empowered, an organization that advocates for people at high genetic risk for breast and ovarian cancer.
Today, she is an outreach coordinator for FORCE, helping link women through face-to-face groups and one-on-one pairings as they face life-altering decisions.
‘It was very hard getting those results,’ said Lisa Stein, a 43-year-old mother of two, who found out she has the gene last year. ‘I was trying to prepare for being positive, but I don’t think you ever can. After I got the results, I really struggled. I was feeling raw for a while, crying easily knowing that it was going to be life-changing.’
Stein’s mother died of breast cancer at 57, and her grandmother died of ovarian cancer, but she didn’t test until her older sister, Lauren Rothman, tested positive.
Rothman opted for a mastectomy, but Stein chose to keep her breasts.
‘I think I knew instinctively that I was not going to have a double mastectomy. That felt too radical to me,’ Stein said. ‘I didn’t feel psychologically prepared or that it was necessary. I don’t feel like cancer is imminent; I feel like I have a few years to take it in and think about it and prepare, so I’ve put that decision on hold.’
She goes in for screening every few months, and she said the anxiety of waiting for those results has been manageable.
Both Rothman and Stein had their ovaries removed, however, which doctors are now recommending for women who test positive and who are finished having children or who are over age 35. Removing ovaries not only reduces the risk of ovarian cancer – which is notoriously hard to catch early and thus has a high mortality rate – but it reduces the risk of breast cancer by 50 percent. Stein also went on Tamoxifen, a drug taken by breast cancer survivors to reduce the risk of recurrence and which reduces risk by 50 percent in BRCA-positive women. The birth control pill, which stops the ovaries from cycling, can also reduce the risk of ovarian cancer but requires more vigilant screening for breast cancer.
Both ovary removal and Tamoxifen push women into menopause, with all its emotional, sexual and physiological ramifications.
‘I think of myself as a healthy person but not like I used to – it’s kind of tainted,’ Stein said. ‘It’s an identity issue. I still think of myself as youthful, but suddenly, I’m dealing with instant menopause, and that doesn’t sit well with me. But I’m dealing with it.’
Stein and Rothman provide support for each other, despite the different routes they’ve taken.
‘I came to reality very quickly – and the reality was I wanted to see my children grow up, and I didn’t want cancer, and I didn’t want chemotherapy. I wanted the rest of my life,’ Rothman said. Her daughters were 3 and 5 years old when she had surgery.
Rothman, a program director for Hadassah of Southern California, traveled to New Orleans for her breast procedure – two surgeries and tatoooing – at a small clinic that specializes in natural-tissue reconstruction, where a solid flap of fat is removed from the belly and inserted into the shell of the breast after tissue has been removed. The surgery offers a more natural result than silicone implants, though it is longer and more involved.
‘This procedure has provided me with a new outlook on life. It has taken a huge weight off my shoulder,’ Rothman said. ‘I no longer go into mammograms thinking, “Is this the year I’m going to get cancer like mom?'”
And she loves her new body – she got not only a breast lift but a bonus tummy tuck, too.
Advances in reconstructive techniques mean that women have several options for maintaining a body they can feel proud of.
Decades ago, radical mastectomies removed all the tissue and muscle of the chest wall. Today, the muscle is not removed, and reconstructive surgery, usually at the time of mastectomy, can leave intact the women’s natural skin, but in most cases the nipples and areola are removed. A silicone implant, or, as in Rothman’s case, fat from the abdomen, fills the pocket from which breast tissue was removed. Nipples and areola are tattooed on, or some surgeons use a new technique that leaves a woman’s own nipple and areola intact. Doctors try to bury scars in the fold beneath the breast, though that is not always possible.
But even the most beautifully done reconstructions leave a woman with scars and no sensation in her breasts.
‘When women come to see me, my approach is to listen to them and find out where they are in life and how they relate to their own breasts,’ said Dr. Kristi Funk, a breast surgeon and director of patient education at Cedars’ Brandman Breast Center. ‘Women have different feelings about sexuality and what roles breasts play, and that makes a big difference.’
Funk also finds out about the woman’s relationship status, and how she has been affected by a family history of cancer.
More information, better treatment
Family histories can be deceptive, however. Some families don’t know their medical histories, because they were lost due to the Holocaust or immigration.
The gene also can hide out in male members of a family.
A BRCA 1 gene mutation raises the risk of male breast cancer to 6 percent, and there is no increased risk for other cancers. BRCA 2 mutation also increases the risk for melanoma, prostate and pancreatic cancer. Still, men who carry the gene are likely never to get any cancer, although they have a 50 percent chance of passing the gene to children. Families with few females may never discern any cancer history.
Dora Cohen (not her real name) suspects it was her father who passed the BRCA 1 gene mutation to her. Last year, she was diagnosed with DCIS, a noninvasive cancer, which was treated with a lumpectomy and radiation. Of the many oncologists she saw, only one recommended that as an Ashkenazi woman in her 40s, she probably should have genetic testing.
In the last six months, Dora has had her ovaries, uterus and breasts removed.
Her daughter, Diane (not her real name), who is 27 and has been married for two years, doesn’t want to get tested yet.
‘I see what my mom is going through,’ Diane said. ‘I want to have kids, and I’m not in a place where I would take those measures [mastectomy and removal of the ovaries]. Knowing I’m positive and having that pressure on me would be something very difficult to live with.’
She and her husband of two years have pushed up their plans for children, and she worries that a positive test could jeopardize her medical insurance, especially because she is self-employed.
Federal and California law provide fairly good protection against genetic discrimination from insurers, stipulating that a genetic predisposition cannot be considered a pre-existing condition. But individual policies are not as well protected as group policies.
Still, genetics experts say much of the fear is overblown. They point out that there has been little litigation involving genetic discrimination, and that the insurance industry is open to the reality that genetic testing can lead to better and more cost-effective treatment. Most insurers cover genetic testing, and some genetic counseling – a rapidly growing field.
‘The genetics community has been struggling to help people understand the importance of talking to someone who knows the nuances of genetic testing,’ said Heather Shappell, a genetic counselor and founder of Informed Medical Decisions, which offers over-the-phone genetic counseling.
‘Genetic tests do not always yield a yes-or-no answer,’ Shappell said, ‘and often doctors aren’t sure how to read the results and guide patients through their decisions.’
In August, Aetna extended full coverage for Shappell’s phone-counseling services to its 14 million policyholders.
What geneticists are looking for is an error in the sequencing of the BRCA gene.
All people carry two genes, BRCA 1 and BRCA 2, which prevent cancer by repairing damaged cells. A mutation damages the genes’ repair function, which leads to uncontrolled growth and causes cells to become cancerous.
About 95 percent of Ashkenazi Jews who have the mutation have one of three errors, which means the mutation is easier to find and the test costs much less – about $400, as compared to $3,000 for a test that analyzes the entire gene.
As researchers learn more about how BRCA mutations cause cancer, they are developing targeted treatments.
A clinical trial with sites at Cedars and City of Hope uses a drug called a PARP-inhibitor to shut down the cell’s backup repair function. Normal cells are not affected, because the primary repair pathway is still functioning. But cancerous cells are left with no functioning repair system, so those cells die. Because normal cells are not affected, there are few major side effects.
‘We have a promising situation where you have a treatment which is completely targeted to cancer and leaves the normal cells alone. And that is very different from treatments like chemotherapy, where there is toxicity to every cell,’ said Audeh of Cedars.
Another study in Israel has found that women with ovarian cancer who are BRCA positive respond better to chemotherapy and have a higher survival rate than women who are not carriers, according to Jeff Weitzel at City of Hope. Weitzel, an investigator in the PARP-inhibitor trial, is also working on a study that manipulates hormones to reduce breast density, which makes surveillance through mammography and ultrasound more effective.
In February, the Jerusalem Post reported that doctors for an Orthodox woman undergoing in-vitro fertilization at Hadassah Hospital were able to identify and screen out embryos that had inherited her BRCA mutation. [Jerusalem Post Feb. 2008 article abstract]
A gift of life?
But while such progressive procedures have been generally well received in Israel, there is still social reluctance to test for the gene, especially in traditional circles, where families fear a genetic flaw could hurt the marriageability of their kids.
Debra Nussbaum Stepen, a Los Angeles therapist who now lives in Israel, is trying to break those perceptions. She works as a therapist at a clinic for hereditary breast and ovarian cancer, and she volunteers for Bracha, a Hebrew-language Web site for BRCA carriers.
The name of the site – bracha means blessing and is a play on BRCA – connotes that knowing one’s genetic makeup is a blessing that can save one’s life.
It is a lesson Stepen learned personally.
Her father had several kinds of cancer, including breast cancer, and before he died at 77, Debra urged him to get genetic testing. She was 51 and had never had cancer when she found out she carried the gene.
‘My doctor told me my breasts were ticking time bombs, and I couldn’t go to bed at night knowing that and thinking today am I going to get cancer?’ said Stepen, who has three stepchildren and a new stepgranddaughter.
She observed her father’s first yahrzeit in New Orleans, where she was undergoing the third and last part of a double mastectomy and reconstruction.
‘I said to my husband, in my father’s death he gave me the gift of life,’ Stepen said.
It takes time to reach this comfort level. As Erika Taylor prepares for her surgery in a few weeks, she worries about the ‘gift’ she may give to her son. She and her mom have talked about how irrational that guilt is.
‘I can say to my mom, “You didn’t know. It’s OK. It’s not your fault,’” she said. ‘But when it comes to me and my son, I think how could I have done this to my son. I am in abject horror that I might have passed this on to him. I know it’s irrational, but the whole idea fills me with grief.’
At the same time, she has hope.
‘My grandmother died from breast cancer at 56. My mother almost died of this disease. And I’m not going to even come close to dying,’ Taylor said. ‘My hope for my son, if he has this, is that he may not have to have any medical intervention at all. Maybe they can repair this mutation. The idea that there is trajectory moving in the right direction gives me some comfort and hope.’”
[Quoted Source: “Jewish women change their destinies by testing for genetic mutation,” by Julie Gruenbaum Fax (Jewish Journal of Greater Los Angeles), Texas Jewish Post, April 24, 2008 (emphasis added)]
Comment: For additional information relating to hereditary breast and ovarian cancer with respect to all women (Jewish and Non-Jewish), refer to the following: (i) FORCE: Facing Our Risk of Cancer Empowered; (ii) National Breast and Ovarian Cancer Coalition; (iii) “Clinical Considerations,” Genetic Risk Assessment and BRCA Mutation Testing for Breast and Ovarian Cancer Susceptibility Recommendation Statement, U.S. Preventive Services Task Force (USPSTF), Agency for Healthcare Research & Quality (AHRQ), U.S. Department of Health & Human Services, September 2005; (iv) “Genetics” hyperlinked materials, H*O*P*E* Blog homepage.